Men are more likely than women to suffer from acute kidney injury, which occurs when kidney function suddenly declines. An experiment with mice suggests that this may be related to having higher testosterone levels.
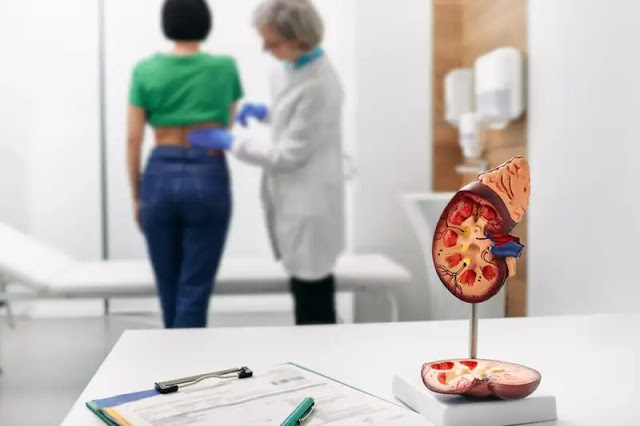 |
| Acute renal damage precipitates an abrupt reduction in kidney function. Shutterstock/Peakstock |
Low testosterone levels appear to protect kidney cells from cell death in mice. The discovery may help to explain why women have a lower risk of acute kidney injury than men.
Tomokazu Souma of Duke University in North Carolina collected and genetically sequenced kidney samples from eight mice, four females and four males. They discovered 128 genes that differed in expression between the sexes, and further investigation revealed that many of these genes were linked to a specific cell process known as NRF2. This process is known to protect against ferroptosis, a type of cell death that is a cause of acute kidney injury in humans, in which the kidneys suddenly lose function.
To see if sex hormones affect NRF2 protection, the researchers removed the ovaries of six female mice and the testicles of four male mice in a separate experiment, so that the mice had less oestrogen and testosterone than normal.
Advertisement
Three to four weeks later, they sequenced the animals' genes and discovered that the procedure had no effect on the NRF2 genes in female mice. When male mice were compared to mice without testicles, the expression of two of the genes - GSTA4 and CBR1 - increased more than fivefold on average.
According to Souma, this suggests that testosterone inhibits the NRF2 process in male mice, making them more susceptible to ferroptosis in their kidneys and possibly explaining why men have higher rates of kidney injury.
However, oestrogen may still play a role in the sex differences in kidney disease. Another study conducted by the team discovered that female mice lacking ovaries had poorer kidney function than those who did.
"Many different mechanisms have been investigated in terms of sex differences in acute kidney injury, and they all appear plausible," says Joel Neugarten of Montefiore Medical Center in New York. "And the difference is most likely explained by a combination of different factors."
Journal citation: Cell Reports, DOI: 10.1016/j.celrep.2022.111610.